What is Revenue Cycle Management in Medical Billing
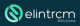
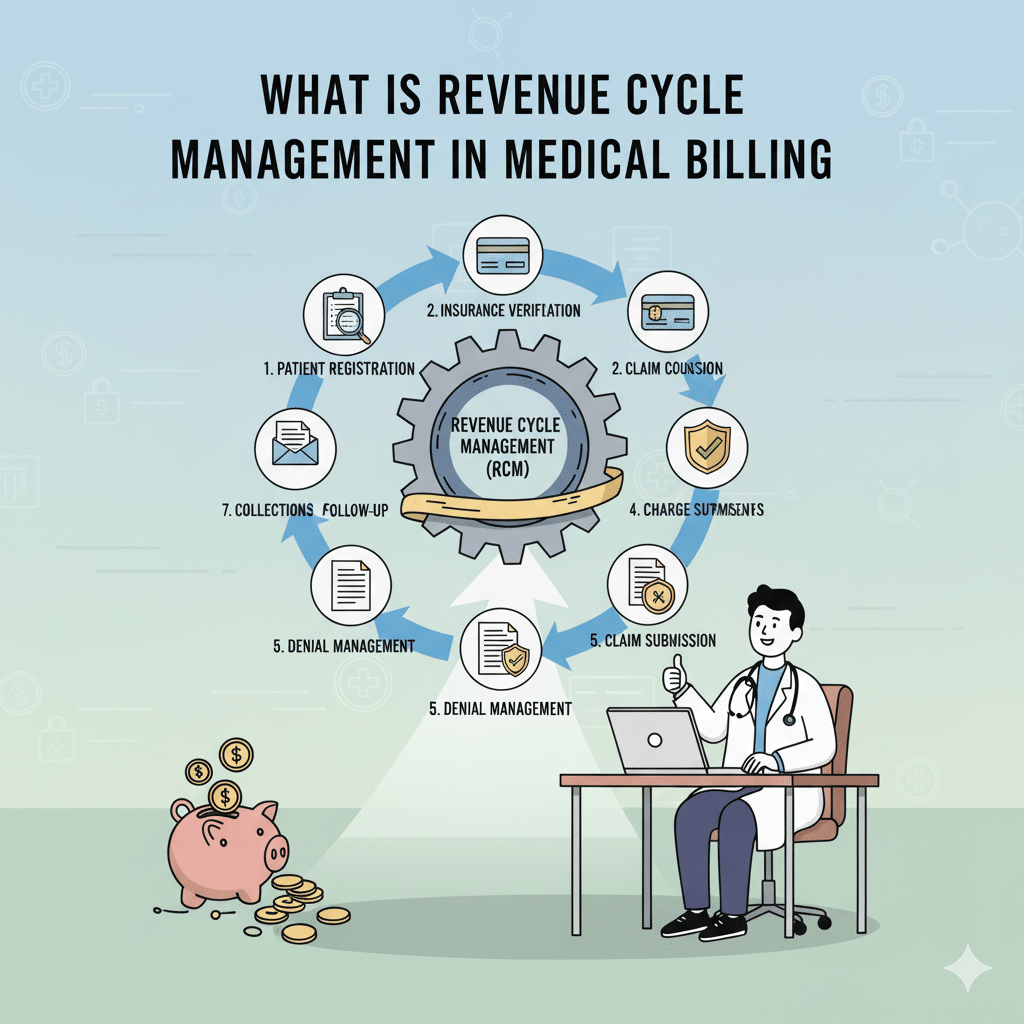
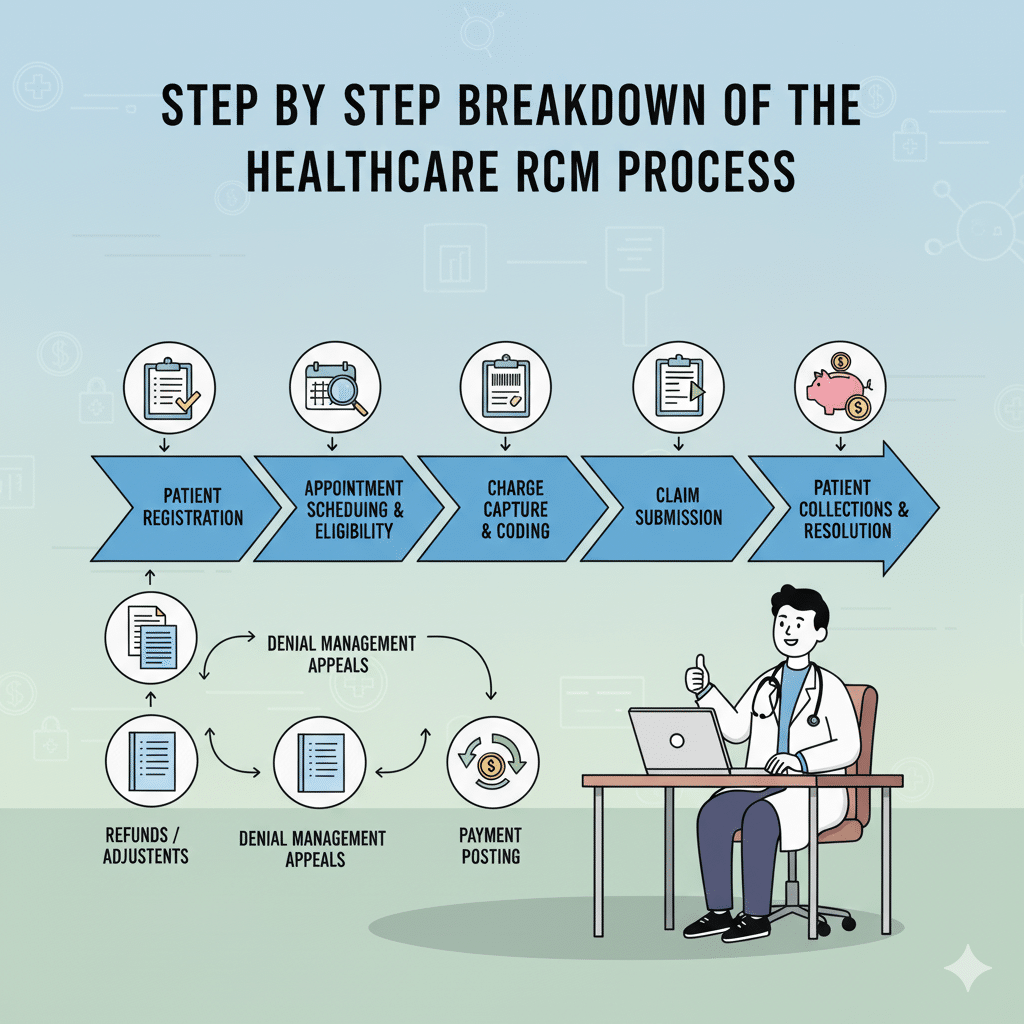
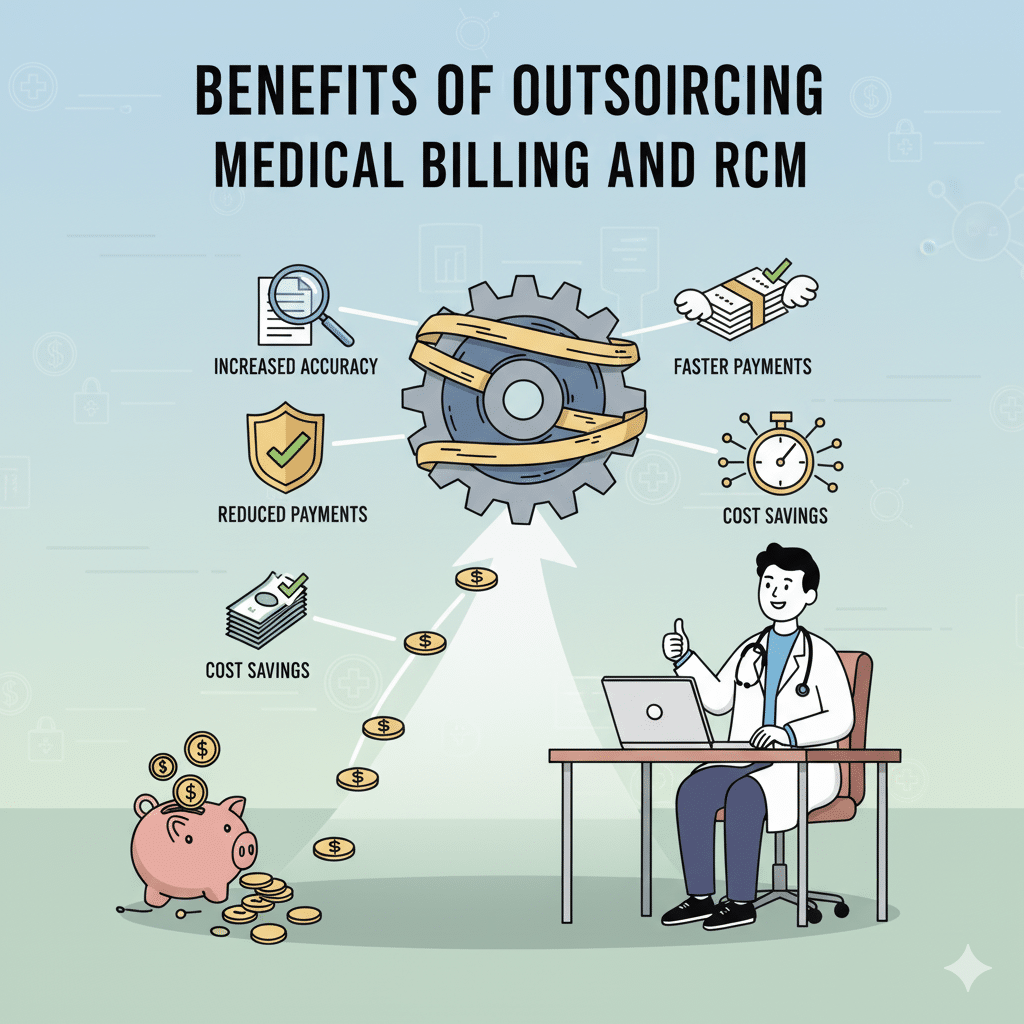
What is Revenue Cycle Management in Medical Billing? In the modern healthcare sector, excellent patient care is just one half of the story. Behind all the medical consultation, diagnosis tests, or even surgeries, there exists a fancy financial procedure that makes sure that the providers are adequately rewarded as a result of their services. This is referred to as Revenue Cycle Management (RCM). RCM is often known as the backbone of healthcare finance and is a combination of administrative work and financial processes. It also guarantees the providers to get prompt payments and reduce claim errors and denials. Despite the most successful healthcare organizations, the lack of an effective RCM system may turn into delayed payments, disruptions in cash flows, and unsatisfied patients. This guide will take you through the fundamentals of RCM in medical billing, the major aspects involved in it, and how a trusted group such as ElintRCM can revolutionize the manner in which healthcare organizations manage their financial activity. Knowledge of Revenue Cycle Management (RCM) Definition of RCM Revenue Cycle Management (RCM) is the total cycle of monitoring and controlling of patient revenue, which begins with the appointment of a patient to the time when all the payments are received. It integrates medical billing, medical coding, insurance verification, claims administration, posting of payment and collections into a single continuous process. Rudimentarily, RCM guarantees that medical practitioners can be paid the correct amount of money they deserve due to the care they offer. RCM is Important in Healthcare RCM is not just about money. It is concerned with efficiency, compliance and sustainability. In case of effective management of RCM processes: First time claims are made in the right way and hence denials are minimized. Professional service providers remain in line with the changing payer rules and regulations. Patients have less unpleasant financial experiences and fewer billing surprises. In the case of healthcare providers, RCM has a direct effect on financial health, operational efficiency, and general trust of the patients. Key Components of RCM RCM consists of numerous interrelated steps. Every step should be dealt with in a way that prevents delays or loss of revenue. Patient Scheduling & Registration This will start when a patient makes an appointment. This will be a critical point in gathering correct demographic and insurance information. Such mistakes as the misspelling of a name or the insurance information that is out of date can multiply to the refusal of claims further into the cycle. Check of Insurance Eligibility It is essential to check the insurance eligibility before the visit. This is done to make sure that the coverage of the patient is valid and makes clear what services will be covered. Lack of eligibility confirmation leads to rejection of claims, payment delays or expensive surprises to patients. Medical Coding & Charge Entry After delivery of the service, it has to be coded into standardized codes (ICD-10, CPT, HCPCS). The most common causes of claim denials include coding errors that could be the use of outdated codes or lack of correspondence in the procedures. The entry of the charges allocates correct charges to these codes, thus, being transparent. Submission and Processing of Claims One of the most important steps is to submit claims to the insurance companies. Here there can be no compromise of accuracy. Absence of modifiers, wrong provider numbers or wrongly matched data may lead to denials. Effective collection of claims raises the rates of first-pass acceptance i.e. claims are approved upon the first submission. Posting & Collections of Payments Payment is made when claims are processed by the insurer. Not every claim gets reimbursed. Others could be underpaid or rejected. During this process, providers should revise, appeal and re- submit claims where necessary. In the case of patient balances, statements are forwarded and collection procedures are enforced in case the payments are outstanding. The Importance of RCM to Healthcare Providers Improved Cash Flow Optimized RCM guarantees a constant stream of income. Providers can save time and decrease errors, which lower abrasions in finance and result in delays in every claim. Reduced Denials One of the largest obstacles of medical billing is claim denials. An effective RCM system is useful in preventing errors prior to filing the claims, which minimizes rejections and wastage of time on claims appeal. Better Patient Experience One of the primary reasons for patient frustration is billing issues. Under streamlined RCM, patients get correct bills, know their insurance covers and do not experience any unequal financial burden. When there is a more streamlined billing procedure, trust and loyalty is increased. Common Challenges in RCM Despite its significance, several providers find RCM a complicated process because they are faced with: A lot of frequent coding changes that complicate compliance. Human mistakes when registering or billing. Complex payer requirements are different among the insurance companies. Expensive overheads incurred due to handling of billing internally. These issues do not only impact on reimbursement, but they also pull staff to patient-related duties. Why Select ElintRCM to Manage Your Revenue Cycle? The in-house management of the healthcare RCM cycle may be time-effective and expensive. This is the reason why it is a popular choice of many providers to outsource medical billing to reliable partners such as ElintRCM. We practice tailored solutions at ElintRCM, which offers specific solutions to the unique needs of hospitals, clinics, and the private practices. Our services include: Proper patient checking-in and insurance checking to avoid denials at the front office. An effective claims management system to enhance first-pass acceptance rates. Analytics and data-driven reporting which provide the providers with an insight into the financial performance. Through collaboration with ElintRCM, medical practitioners will be able to: Reduce operational costs. Improve collections and profitability. Remain in line with emerging laws. Release personnel to be more effective in patient care, not paperwork. Conclusion Medical billing is not simply a back-office activity as far as Revenue Cycle Management is concerned. It is the bread-winner of healthcare establishments. From patient registration to collecting